For adults with obsessive-compulsive disorder who have not found sufficient relief from medication and therapy, TMS is an FDA-cleared and effective treatment option. Clinical evidence indicates a response rate between 38% and 58%, offering a non-invasive neuromodulation path for treatment-resistant cases.
This article will detail the science, the realistic outcomes, and the specific patient profile for which this intervention is designed. Continue reading to understand if this targeted approach could be the next logical step in your care.
Key Takeaways
- TMS directly modulates brain circuits in the anterior cingulate cortex and medial prefrontal cortex that are linked to OCD symptoms.
- Clinical response rates range from about 38% in rigorous trials to over 50% in real-world practice.
- It is primarily used for adults with clearly documented, treatment-resistant OCD.
The Science Behind Targeting the OCD Brain
In psychiatric practice, there is a particular kind of fatigue that appears in some patients. It is not physical exhaustion, but a gradual wearing down of hope. You see this in adults who have tried different serotonin reuptake inhibitors.
They take the right doses and stick to the treatment for the right time. They also complete structured exposure and response prevention therapy. Still, their days are filled with intrusive thoughts and long, time-consuming rituals.
For this group, TMS offers a different type of intervention. It’s a physical treatment for a mental health condition. It doesn’t use medication or talk therapy. Instead, it relies on electromagnetic induction. Its role isn’t a cure.
Instead, it helps change the activity of overactive brain circuits. This gives some patients a chance to shift a chronic, resistant illness.
The Neurological Target of TMS Therapy

The rationale for using TMS in OCD comes from what we know about the disorder’s brain circuitry. Functional imaging studies repeatedly show increased activity in specific cortical and subcortical regions in people with OCD.
The anterior cingulate cortex (ACC) and medial prefrontal cortex (mPFC) are especially involved. [1]
These regions play key roles in:
- Error detection
- Conflict monitoring
- Feelings of “something is wrong”
- Anxiety and distress signals
In OCD, this network can become stuck in a loop, constantly signaling danger or incompleteness and driving compulsive behaviors as a “corrective” response.
Standard TMS coils (often figure-8 coils) mainly stimulate the outer layers of the cortex. For OCD, deeper structures are involved, so a different approach is needed. The FDA-cleared protocol for OCD uses a Deep TMS coil, called an H-coil.
This design allows the magnetic field to reach several centimeters deeper into the brain, including the ACC and mPFC, with greater precision.
A few key points:
- The treatment does not destroy brain tissue.
- It does not require surgery or anesthesia.
- It uses repeated magnetic pulses to induce longer-term changes in how neurons fire within these overactive circuits.
You can think of it as helping an overactive pathway become less reactive and more regulated, rather than changing the brain’s anatomy.
Key facts about the target:
- The anterior cingulate cortex is a primary TMS target in OCD.
- Deep TMS coils are engineered to reach structures several centimeters below the surface.
- The aim is neuromodulation, not permanent structural change.
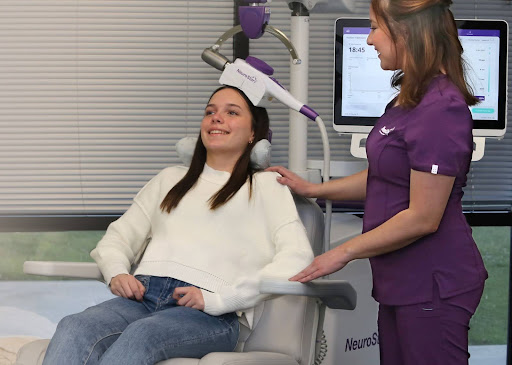
What a TMS Session Looks Like
A TMS session is an outpatient procedure. It’s usually simple for the patient. At a center such as TMS of the Carolina, the process typically looks like this:
- The patient sits in a comfortable chair.
- Using head measurements and standard anatomical landmarks, a trained technician positions the TMS coil against the scalp, following protocols used in neurostar advanced TMS therapy to ensure consistent and precise stimulation.
- The device creates a focused magnetic field. This field goes through the skull and causes a small electrical current in the targeted brain area.
A typical OCD session:
- Lasts about 18 to 20 minutes.
- Requires no sedation.
- Allows the patient to remain fully awake and communicative.
Patients usually report a tapping or knocking sensation on the scalp during stimulation. After the session, they can return to normal daily activities, work, driving, and family responsibilities, without a recovery period. This feature clearly distinguishes TMS from more invasive options like neurosurgery or procedures requiring anesthesia.
What the Response Rates Actually Mean
When we talk about “how effective” TMS is, we are talking about probabilities, not guarantees.
Evidence from Clinical Trials
Randomized controlled trials of Deep TMS for OCD, which led to FDA clearance, show a response rate of about 38%.
In these studies, a “responder” is usually defined as:
- A 30% or greater reduction in scores on the Yale-Brown Obsessive Compulsive Scale (Y-BOCS), the standard tool used to measure OCD severity.
These are not mild cases. Participants generally had moderate to severe, treatment-resistant OCD, meaning they had already tried multiple medications and therapy without adequate relief. For this group, a greater than 1-in-3 chance of meaningful symptom reduction after exhausting standard options is clinically significant.
Real-World Clinical Practice
In actual clinical settings, reported response rates are often higher, commonly in the 52 to 58% range. This gap between trial data and real-world outcomes is not unusual.
Several factors may contribute:
- Clinicians can individualize or fine-tune protocols within safe parameters.
- Patients may receive better integration with ongoing treatments (medications, therapy).
- Comorbid conditions like major depressive disorder (MDD), for which TMS is also FDA-cleared, may improve at the same time, amplifying the benefit.
Time Course of Improvement
Improvement is usually gradual, not immediate:
- Subtle changes often emerge in weeks 3 to 4 of a standard 6-week course.
- Gains may continue to build in the weeks following the completion of daily sessions.
Many patients describe:
- Less intensity or frequency of obsessions.
- Reduced urgency to perform compulsions.
- Slightly more “space” between the intrusive thought and the need to act.
Durability and Maintenance
How long the benefit lasts is still being studied, but current experience suggests:
- Many patients maintain gains for months after the initial course.
- Some patients benefit from maintenance sessions (for example, every few weeks or months) to prolong the effects.
This is similar to maintenance approaches used in other chronic medical conditions. Ongoing neuromodulation doesn’t mean failure; it shows the long-term, biological aspect of OCD.
The main goal is to build a stable baseline. This helps patients and their therapists manage remaining symptoms better.
Protocol Specifics: More Than Just a Magnet

TMS for OCD is not simply “turning on a magnet.” The FDA-cleared protocol includes several key features that are important to understand, particularly within structured approaches to TMS therapy for OCD that emphasize precision and consistency. [2]
Symptom Provocation
One distinctive component is symptom provocation immediately before the TMS session.
- The clinician briefly discusses or triggers a mild exposure related to the patient’s main obsession or compulsion.
- The purpose is to activate the OCD circuit right before stimulation.
Engaging the specific network being targeted can make TMS pulses more effective. This leads to a stronger and more precise neuromodulatory effect. The goal is not to cause extra stress. Instead, we aim to make the treatment more precise and effective at the circuit level.
Stimulation Parameters
The OCD protocol is carefully defined:
- High-frequency stimulation, typically 20 Hz
- Targeted to the medial prefrontal cortex/anterior cingulate region
- Daily sessions, 5 days per week, for 6 weeks (acute course)
Consistent stimulation is key for lasting changes in how circuits function. This process is known as neuroplasticity. The schedule needs commitment. The treatment is non-invasive. So, it fits into daily life better than many intensive medical options.
Safety and Side Effects
TMS has a good safety profile. This is especially true when compared to systemic medications or surgeries.
| Category | Details |
| Common Side Effects | Scalp discomfort, mild headache |
| Typical Duration | Transient; resolves after treatment |
| Systemic Side Effects | None (no weight gain, sexual dysfunction, or sedation) |
| Serious Risks | Seizure (rare, <1% with proper screening) |
| Pre-Treatment Screening | Seizure history, neurological conditions, metal implants |
Before starting, a physician conducts a thorough screening to look for:
- Personal or family history of seizures
- Neurological conditions
- Medications that may lower seizure threshold
- Any metal or implants that might interact with the magnetic field
Key protocol points:
- Symptom provocation is a required part of the FDA-cleared OCD protocol.
- Treatment uses 20 Hz high-frequency stimulation, daily for 6 weeks.
- Most side effects are mild and localized (scalp discomfort, headache).
Determining Your Candidacy for TMS Therapy

TMS is not a first-line treatment for OCD. It is designed for adults with treatment-resistant illness, aligning with clinical criteria used in structured TMS therapy for OCD programs.
In practice, that usually means:
- You are 18 or older with a confirmed diagnosis of OCD.
- You have not responded well to at least two serotonin reuptake inhibitors (SRIs) at the right doses and for the right time.
- You have completed a course of evidence-based psychotherapy, especially exposure and response prevention (ERP), without adequate relief.
These criteria help find people who can benefit from TMS, making the time and cost worthwhile.
Medical Contraindications
TMS is contraindicated in patients with:
- Ferromagnetic metal in or near the head (excluding the mouth), such as:
- Certain aneurysm clips
- Some stents
- Implanted electrodes
- Cochlear implants
- Implanted electronic devices that could malfunction in a magnetic field
- Some active neurological conditions or unstable seizure disorders
A detailed medical history and, if needed, a neurologic evaluation help assess safety.
Insurance and Access
For patients who meet criteria, TMS is covered by many major insurance plans, including Medicare, when used for approved indications and when documentation of treatment resistance is provided.
The treating clinic usually assists with:
- Prior authorization
- Submission of records showing previous medication and therapy trials
Comorbid Depression
Many adults with OCD also have major depressive disorder (MDD). This does not disqualify someone from TMS; in fact, it can strengthen the case for treatment.
Devices such as NeuroStar Advanced Therapy are FDA-cleared for both OCD and MDD. Treating both conditions with the same neuromodulation approach can:
- Improve mood
- Reduce overall distress
- Potentially enhance engagement with ERP and other therapies
TMS is an add-on, not a substitute, for medication and therapy. Ideally, it is integrated into a broader, coordinated treatment plan.
A Clinical Perspective on Neuromodulation
TMS for obsessive-compulsive disorder is supported by clinical research and a clear neurobiological framework. For adults with documented, treatment-resistant OCD, it offers roughly a 38 to 58% chance of meaningful symptom reduction.
Key strengths include non-invasive outpatient delivery, minimal systemic side effects, and direct targeting of brain circuits medications may not reach. TMS does not replace standard care, but it offers an evidence-based next step. To explore whether this option fits your needs, schedule a consultation here.
References
- https://pubmed.ncbi.nlm.nih.gov/36740349/
- https://pubmed.ncbi.nlm.nih.gov/35990054/
