Article description: Wondering “Does TMS work for anxiety?” Explore how this treatment reduces symptoms, supports recovery, and helps people regain control of their daily life.
Transcranial Magnetic Stimulation, or TMS, is a non-invasive treatment cleared by the FDA that targets nerve cells in the brain to help reduce anxiety symptoms. For many who struggle with anxiety, traditional methods like medication or therapy don’t always bring relief.
TMS offers a different approach by using magnetic pulses to stimulate areas of the brain that may be underactive in anxiety disorders. Studies and clinical use suggest it can make a real difference, especially when other treatments fall short. If you’re curious about how TMS works and whether it might help, keep reading.
Key Takeaways
- TMS targets the prefrontal cortex to calm overactive anxiety circuits in the brain.
- Clinical studies show significant anxiety reduction, especially for treatment-resistant cases.
- The treatment is non-systemic, meaning no body-wide side effects like those sometimes seen with medication.
What is TMS and How Does It Affect Anxiety?
Anxiety can be understood as the brain’s alarm system stuck in the “on” position. Transcranial Magnetic Stimulation (TMS) is a non-invasive treatment designed to reset this system.
It uses focused magnetic pulses, like those in an MRI, to stimulate specific brain areas involved in mood and anxiety control. Unlike medications that affect the whole body, TMS targets the brain directly.
The main area targeted in anxiety treatment is the dorsolateral prefrontal cortex (DLPFC). This region helps regulate emotional responses. In anxiety, the connection between the DLPFC and the amygdala,the brain’s fear center,can weaken. TMS gently stimulates the DLPFC, which may strengthen its control over the amygdala, reducing excessive worry and fear.
This method is important because it offers an option when medications or therapy don’t provide enough relief. For patients who have not responded well to antidepressants or cognitive-behavioral therapy, TMS offers a treatment based on brain biology without sedation or widespread drug effects.
- Targeted Stimulation: Magnetic pulses are focused precisely on the prefrontal cortex.
- Neuromodulation: The goal is to modulate, or rebalance, neural activity in key circuits.
- Non-Invasive: There are no incisions, and the procedure is performed while you are awake.
How TMS Reduces Anxiety Symptoms: The Science

Transcranial Magnetic Stimulation (TMS) works through a process called neuromodulation. Instead of using medication, TMS uses electromagnetic induction to create small electrical currents in the brain.
These currents can either increase or decrease nerve cell activity, depending on the frequency of the magnetic pulses. For anxiety, high-frequency pulses are typically applied to the left dorsolateral prefrontal cortex (DLPFC). This stimulation activates an underactive brain region involved in emotional regulation.
By increasing activity in the left DLPFC, TMS helps improve its control over the amygdala, the brain’s fear center. When the amygdala calms down, symptoms such as rapid heartbeat, muscle tension, and persistent worry often decrease.
Patients often report feeling calmer and more in control. The brain’s circuits are not damaged but out of balance; TMS aims to restore this balance.
Research supports these effects. Brain imaging before and after TMS shows increased activity in the prefrontal cortex and reduced overactivity in the amygdala.
These changes correspond with the symptom relief patients experience. TMS directly influences the neural pathways involved in anxiety.
Anxiety can be thought of as a “persistent alarm system” that is overly sensitive, sending false danger signals. TMS helps reset this alarm by teaching the brain to respond more appropriately, not by sedating it. With repeated sessions, the brain gradually learns a calmer, less anxious state.
This process depends on neuroplasticity,the brain’s ability to reorganize by forming new connections. TMS encourages this rewiring, like how physical therapy helps muscles heal. With ongoing treatment, brain function improves steadily and sustainably.
What the Research Says: TMS Efficacy for Anxiety

The evidence supporting TMS for anxiety is growing. Many studies have used standard tools like the Hamilton Anxiety Rating Scale (HAM-A) to measure how well it works. These studies show that patients who receive real TMS treatment have bigger drops in anxiety symptoms than those who get a placebo.
A meta-analysis involving 152 adults with Generalized Anxiety Disorder reported a large symptom reduction, with an effect size of SMD-1.857, indicating strong clinical improvement for those receiving active TMS compared with sham [1].
In Generalized Anxiety Disorder (GAD), where people worry a lot and can’t control it, TMS aimed at the dorsolateral prefrontal cortex (DLPFC) has shown clear benefits.
These improvements are measured by doctors, not just reported by patients. Similar results are seen in Post-Traumatic Stress Disorder (PTSD), where TMS helps reduce symptoms like feeling overly alert or having flashbacks.
TMS is cleared by the FDA for depression and obsessive-compulsive disorder. Using it for anxiety is off-label but backed by strong research.
Off-label use is common in medicine when studies show a treatment helps beyond its original approval, especially when clinicians use established systems such as NeuroStar Advanced TMS Therapy. Doctors decide to use TMS for anxiety based on this evidence and patient needs.
The effects of TMS usually last. Follow-up studies show that symptom relief can continue for months after treatment ends. For many people with long-lasting anxiety that hasn’t improved with other treatments, TMS offers a lasting option.
What to Expect: TMS Treatment Protocol and Duration
A typical TMS treatment follows a clear and consistent schedule. If you’re considering TMS, expect a commitment like physical therapy. The first step is a mapping session.
During this appointment, the technician locates your motor cortex to precisely position the TMS coil. This ensures the magnetic pulses target the prefrontal cortex accurately.
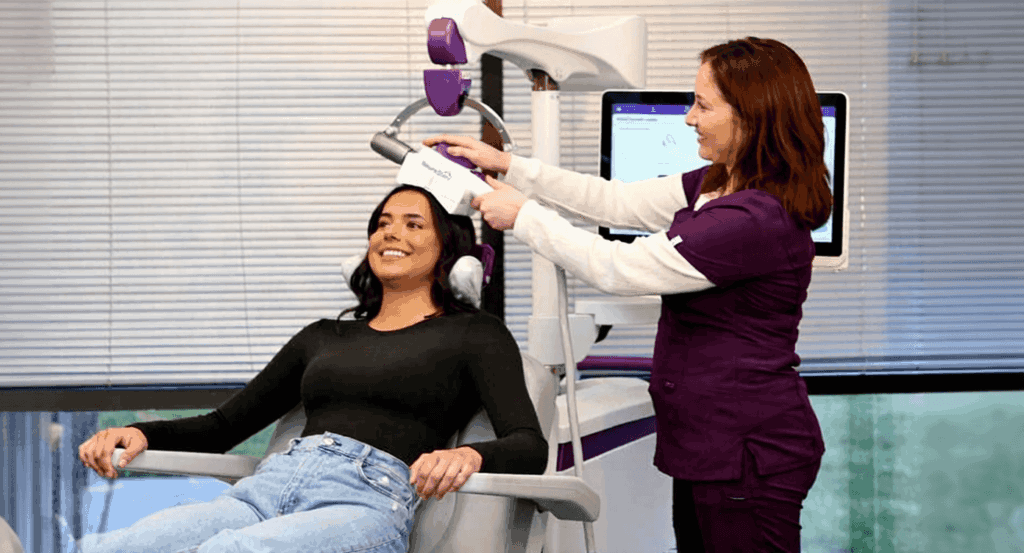
Treatments take place in an outpatient setting. You remain awake and seated comfortably for about 20 to 30 minutes per session. The coil rests against your head, producing clicking sounds and a tapping sensation on your scalp.
You can relax, listen to music, or watch TV during the procedure. There is no downtime,you can drive yourself home and return to normal activities right away.
Typically, treatment involves sessions five days a week for four to six weeks. This schedule helps build the cumulative effect needed for lasting changes in brain activity.
The total number of sessions varies depending on individual response and the protocol used. Some newer methods, like Theta Burst Stimulation, reduce session time to about three minutes, making treatment easier to fit into busy lives.
- Frequency: Typically 5 sessions per week.
- Duration: Each session lasts 20-30 minutes (or 3 minutes for express protocols).
- Course Length: A full treatment course generally spans 4 to 6 weeks.
The specific TMS coil used can also influence the treatment. Different coils have varying depths and patterns of magnetic field penetration.
A specialist will choose the appropriate equipment based on the treatment target and individual anatomy. Throughout the process, the treatment team monitors your progress and adjusts parameters as needed to optimize outcomes.
Potential Side Effects and Safety of TMS for Anxiety
TMS has a strong safety record. Because it is non-invasive and does not require anesthesia or systemic drugs, the risks are much lower than with more invasive treatments.
Most side effects are mild and short-lived, usually happening during or soon after a session. In a broader safety review of TMS studies, researchers found no severe adverse events and noted that dropout rates were similar between TMS and control groups, reinforcing its strong safety profile [2].
The most common side effect is a mild headache or scalp discomfort where the coil touches the head. This often feels like a tension headache and usually goes away on its own or with over-the-counter pain medication. Some patients may notice brief lightheadedness or facial twitching during treatment. These effects are temporary and usually fade after the first few sessions.
Serious complications are very rare. The main concern is the small chance of a seizure, but this risk is less than 0.1% when safety guidelines are followed. Before treatment, providers carefully screen patients for factors that could increase seizure risk, such as a personal or family history of epilepsy or certain neurological conditions.
Because TMS does not involve sedation or cognitive impairment, most patients are able to resume normal daily activities, including driving themselves to and from TMS appointments, immediately after each session. This is an important distinction compared to other interventional mental health treatments.
It is important to consult a qualified healthcare professional before starting TMS. They will check for any contraindications, like non-removable metal in the head (such as aneurysm clips or stents) or implanted devices like deep brain stimulators or cochlear implants. For most patients, TMS is a safe and well-tolerated option with fewer side effects than long-term medication use.
TMS vs. Other Anxiety Treatments: A Comparison
Knowing where TMS fits among anxiety treatments is key to making a clear choice. The first-line options usually include psychotherapy, like Cognitive Behavioral Therapy (CBT), and medications such as antidepressants or anti-anxiety drugs. These treatments work well for many people. TMS is not meant to replace them but offers an alternative when these methods don’t provide enough relief.
TMS’s main advantage is its precision. Unlike medications that affect the whole body, TMS targets specific brain regions involved in anxiety.
This means fewer side effects, no weight gain, sexual problems, or digestive issues often linked to psychiatric drugs. Many people explore clinically guided programs like TMS therapy for anxiety for this reason. TMS also does not cause physical dependence or withdrawal symptoms.
Psychotherapy and TMS work differently. Therapy teaches skills to manage anxiety, while TMS changes the brain’s activity at a biological level. Often, these treatments complement each other. TMS may reduce brain hyperactivity, making it easier for patients to benefit from therapy.
One drawback of TMS is the time needed. Daily sessions over several weeks need a significant commitment. Insurance coverage for TMS in primary anxiety cases is not universal but is improving as research supports its use.
Typically, TMS is offered to patients who have tried one or two antidepressants without success,known as treatment-resistant anxiety or depression.
Real-World Outcomes: Patient Experiences with TMS for Anxiety

The effects of TMS go beyond what clinical scales measure,they show up in everyday life. Many patients report less physical tension, especially in the shoulders and neck. The common sensation of a “knot in the stomach” often eases. Sleep improves as racing thoughts that disrupt rest begin to calm.
Concentration also tends to get better. Anxiety can break focus, making work or conversations difficult. As treatment continues, patients often experience clearer thinking and a stronger ability to stay present.
This can improve job performance and make social interactions less stressful, a pattern also reflected in structured programs such as TMS therapy for adolescents where emotional regulation gains are frequently emphasized.
One of the most important changes is in emotional control. Patients frequently say they feel less reactive.
Situations that once triggered intense anxiety become easier to handle. They gain more control over their emotions instead of feeling overwhelmed by them. This shift can greatly enhance relationships and quality of life, helping people engage more fully in what matters to them.
FAQ
What should I know before trying Transcranial magnetic stimulation anxiety care?
Many people ask how anxiety disorder brain circuits respond to Transcranial magnetic stimulation anxiety care. This method uses noninvasive anxiety treatment steps to guide TMS brain stimulation anxiety activity.
It may help calm the persistent anxiety symptoms TMS tries to target. You can also ask about TMS side effects, anxiety concerns, treatment goals, and what improvement looks like for you.
How does TMS for generalized anxiety disorder compare to other options?
Some people look at TMS for generalized anxiety disorder because they want non-medication anxiety treatments. Repetitive TMS anxiety therapy focuses on anxiety neural activity rebalancing and prefrontal cortex stimulation anxiety patterns.
You may compare TMS depression and anxiety overlap, neuromodulation anxiety treatment choices, and anxiety disorder treatment alternatives to see what matches your symptoms and comfort level.
What should I expect during TMS sessions anxiety disorder treatment?
During TMS sessions anxiety disorder care, a clinician uses magnetic pulse therapy anxiety tools on specific TMS anxiety disorder brain targets.
Many follow a TMS treatment protocol anxiety plan that explains session length and TMS treatment frequency anxiety expectations. People often ask about TMS emotional regulation anxiety changes, anxiety sleep improvement TMS results, and typical TMS therapy duration anxiety experiences.
How do researchers study TMS efficacy anxiety symptoms?
Researchers look at TMS efficacy anxiety symptoms through clinical trials TMS anxiety reviews and anxiety treatment research TMS findings. These studies explore amygdala hyperactivity anxiety TMS responses, TMS anxiety neuroplasticity shifts, and anxiety disorder neuromodulation techniques.
They also check TMS anxiety long-term effects, TMS safety anxiety treatment data, and anxiety patient treatment experience reports to understand how well the method works.
What factors shape anxiety treatment with TMS outcomes?
People often ask how anxiety treatment with TMS supports anxiety symptom relief TMS goals. Factors include anxiety and mood regulation, TMS effects, anxiety concentration improvement, TMS changes, and TMS anxiety muscle tension relief.
Some explore deep TMS anxiety treatment, anxious depression TMS treatment, and TMS as adjunct anxiety treatment. Others review anxiety brain stimulation alternatives and anxiety treatment magnetic stimulation guidelines for clarity.
Finding Your Path Forward with TMS
Deciding if TMS is right for your anxiety begins with a consultation with a specialist. Ideal candidates are adults with persistent anxiety who haven’t found relief from medication or therapy.
The specialist will review your medical history to ensure TMS is safe for you.
Choose a clinic with experienced staff and ask about their TMS system, anxiety treatment experience, and insurance support. Though TMS for anxiety is off-label, many insurance plans cover it, and payment plans may be available.
For a safe, drug-free option, consider NeuroStar Advanced TMS Therapy. Schedule your free consultation with TMS of the Carolinas today.
References
- https://academic.oup.com/ijnp/article/25/2/144/6427794
- https://pubmed.ncbi.nlm.nih.gov/31673675/
