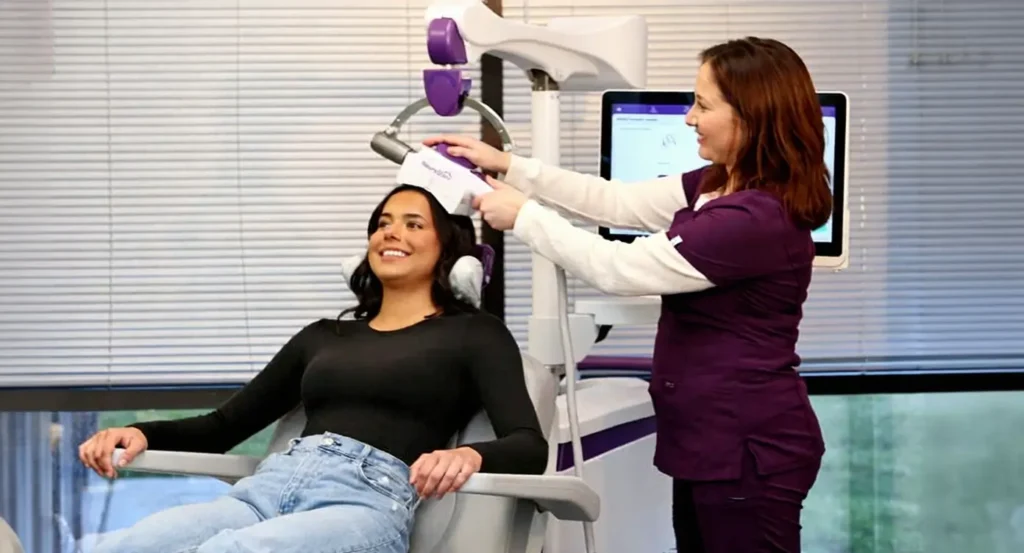
TMS offers a direct way to stimulate mood‑related brain circuits when medication no longer brings relief. The treatment uses magnetic pulses to create small electrical currents in targeted regions, avoiding the need for pills.
Sessions take place in an outpatient chair while a coil rests against the scalp and delivers painless pulses for about 37 minutes. Patients usually leave the clinic and return to regular tasks without recovery time.
For people worn down by repeated medication trials, TMS provides a clear alternative that might guide the next step in care. If you want to understand how it works, keep reading.
Key Takeaway
- TMS offers people with treatment‑resistant depression and obsessive compulsive disorder a non‑invasive option that has FDA clearance.
- Side effects are usually mild, so patients continue their day with little disruption.
- Research shows strong response rates and lasting improvement when the full treatment plan is completed.
What is TMS and Why Does It Matter?
TMS uses focused magnetic pulses to wake up brain circuits tied to mood and motivation. These circuits can slow down during depression, and the pulses help them fire again.
Unlike medication that moves through the whole body, TMS targets the dorsolateral prefrontal cortex, a region linked to mood control. This direct focus reduces the body‑wide side effects that many people feel with antidepressants.
The therapy is done in the office without sedation. You sit still while an electromagnetic coil sends brief pulses through the scalp, and once the mapping is set, the process becomes simple to follow.
A standard session lasts about 19 minutes and happens five days a week over several weeks. Because TMS is non‑invasive, patients leave the clinic and continue with school, work, or home responsibilities right away.
Several features support how well it works:
- NeuroStar’s system offers real‑time feedback and mapping to place the coil accurately.
- Treatment plans adjust to the patient’s own brain activity.
- TMS is often used for major depressive disorder (MDD), obsessive compulsive disorder (OCD), and anxious depression that doesn’t respond to medication.
From a clinical view, TMS helps many people who haven’t found relief with several antidepressants. We see patients find improvement after long periods of frustration, and the therapy stands as a steady option rather than a last hope.
Non Invasive and Safe Alternative

Sometimes depression treatment helps the mind but makes the body feel punished.
Traditional treatment for severe depression can include invasive procedures or electroconvulsive therapy (ECT). ECT needs anesthesia and can bring strong side effects. TMS works in a different way.
TMS does not require surgery or anesthesia. During each session, the patient stays awake and alert. There is no need for a breathing tube, no recovery room, and no waiting for anesthesia to wear off.
Most people feel only mild discomfort. This might be a little scalp tenderness where the magnet rests, or a light headache that usually fades after the session, especially in patients receiving care through structured programs like TMS therapy for depression.
Thinking and memory stay clear. TMS does not interfere with how someone remembers, focuses, or solves problems.
Because TMS does not use medicine that spreads through the whole body, it can be helpful for people who have had:
- Bad reactions to antidepressants
- Weight gain from medication
- Ongoing exhaustion
- Stomach or digestion problems
Over many years of clinical use, the safety of TMS has been carefully documented. That record makes it a serious option for patients who feel limited by medication side effects.
TMS sits outside what traditional treatments demand from the body, and that difference can matter a great deal when someone has already struggled to tolerate pharmaceutical treatment.
Effective for Treatment Resistant Depression

When standard antidepressants and therapy don’t work, treatment resistant depression becomes a real problem that needs a different approach. NeuroStar’s TMS therapy, which the FDA has cleared, has actually shown strong results for these patients.
The numbers from large clinical studies are worth paying attention to:
- About 83% of patients respond to TMS.
- Around 62% go into remission that means their symptoms get substantially better.
- These results come from patients who tried multiple medications first and didn’t get better.
Why does TMS work this way? The therapy works by changing how electrical activity moves through the brain, essentially resetting circuits that aren’t functioning right. Now, doctors don’t usually start with TMS as a first option. It’s something we consider after medications have already been tried and haven’t worked.
Minimal Systemic Side Effects
Transcranial magnetic stimulation works differently from pills. The magnetic pulses target specific brain regions rather than traveling through the bloodstream to affect the entire body. This targeted approach means fewer unwanted effects overall.
Patients don’t experience the side effects common with antidepressant medications. No sedation. No sexual dysfunction. No withdrawal symptoms when treatment ends. What most people do report is mild, temporary discomfort at the scalp where the coil sits, and even that tends to fade quickly.
The practical benefit here matters. Patients can return to their daily routines right after sessions, whether that’s work, classes, or family responsibilities. They’re not dealing with drowsiness or the other complications that sometimes make medication management difficult.
Throughout the entire course of treatment, the clinical team at TMS of the Carolinas observes each patient closely. We track how they’re responding, adjust settings if needed, and address any concerns that come up. The goal is straightforward: deliver effective treatment while keeping discomfort to an absolute minimum.
Improves Mood and Cognitive Functions
Depression and anxiety don’t just affect mood, they actually interfere with how the brain handles concentration, memory, and the kind of thinking needed to get through a day. TMS therapy addresses this in a meaningful way. It reduces mood symptoms, sure, but it also seems to help people think more clearly.
What we’re seeing in studies:
- Enhanced attention span. Patients report they can actually focus on a task without their mind wandering as much.
- Better working memory. They hold information in mind more effectively which matters when you’re trying to follow a conversation or complete a multi step task.
- Improved problem solving ability. The kind of flexible thinking required to work through problems, rather than getting stuck in a loop, improves noticeably.
When these cognitive improvements happen, something shifts. Patients don’t just feel better emotionally, they actually function better. They’re more present with their families, more reliable at work, less likely to withdraw from the people around them. That difference between symptom relief alone and cognitive recovery is what really changes how someone lives their life after treatment.
Potential for Other Conditions
NeuroStar carries FDA clearance for major depression, OCD, and anxious depression, but the research into transcranial magnetic stimulation stretches beyond these diagnoses. Scientists have begun studying TMS in other psychiatric and neurological conditions, and what they’re finding is worth paying attention to.
The evidence is still preliminary, but it points toward some real possibilities:
- Generalized anxiety disorder (GAD) patients with persistent worry and tension show measurable shifts in brain activity after treatment.
- Post traumatic stress disorder (PTSD) early studies suggest TMS may help interrupt the neural patterns that keep trauma responses locked in place.
- Bipolar disorder though this requires more caution than other conditions, researchers are exploring how TMS might work alongside mood stabilizers.
- Chronic pain syndromes connected to mood disorders the brain’s pain processing centers seem to respond to magnetic stimulation in ways that reduce suffering.
Here’s what matters: these applications remain investigational.
A clinician needs to evaluate each patient individually, weighing the evidence, the patient’s medical history, and what other treatments have already been tried, especially when age-related considerations come up, such as the age cut off for TMS is.
There’s no one size fits all approach here. The theoretical promise is there, but clinical judgment comes first.
Promotes Neuroplasticity and Brain Recovery
Sometimes a treatment starts in one area, then slowly begins to touch many others. TMS looks a bit like that right now.
NeuroStar has FDA clearance for:
- Major depression
- Obsessive‑compulsive disorder (OCD)
- Anxious depression
Those are the approved uses today.
But research on transcranial magnetic stimulation goes beyond these. Scientists are testing TMS in other mental and brain conditions, and the early results are interesting, even if they’re not final yet.
Some areas being studied:
- Generalized anxiety disorder (GAD): people who live with constant worry and body tension have shown measurable changes in brain activity after TMS sessions.
- Post‑traumatic stress disorder (PTSD): early studies suggest TMS might help break the brain patterns that keep trauma reactions stuck.
- Bipolar disorder: this area needs extra care, but researchers are looking at how TMS could work together with mood stabilizer medicines.
- Chronic pain tied to mood problems: the brain’s pain centers seem to respond to magnetic pulses in ways that may lower the sense of pain.
All of these uses are still being tested. They are called “investigational” because they are not firmly proven or officially approved for these conditions.
So each patient needs:
- A careful review by a clinician
- Attention to medical and mental health history
- A check of what treatments have already been tried
There is no single plan that fits everyone. The science behind these new uses is promising, but real‑world decisions still have to be guided by clinical judgment first.
Convenient Outpatient Treatment
NeuroStar TMS therapy is delivered on an outpatient basis. Patients typically undergo sessions five days a week for six to seven weeks.
- No hospital stay required. The procedure happens in a clinic setting, meaning you walk in, get treated, and walk back out the same day.
- No anesthesia means no recovery time. Since we’re not putting you under, your body doesn’t need to wake up and adjust afterward. Your mind stays sharp throughout.
- Patients resume normal activities immediately. You can drive yourself home, go back to work, or grab lunch with a friend right after your session ends.
This convenience helps maintain life routines, reducing treatment barriers. When treatment fits into your existing schedule rather than disrupting it, you’re more likely to stick with the full course. That consistency matters for outcomes.
Is TMS Right For You? A Quick Checklist
Consider TMS if:
- You’ve tried several antidepressant medications and they haven’t worked. Major depressive disorder can be stubborn that way, and sometimes the standard approach doesn’t stick. [1]
- You’re dealing with side effects from antidepressants that make life harder instead of better. Nausea, weight gain, sexual dysfunction aren’t small inconveniences, and they matter when you’re trying to get well.
- You’d rather explore something that doesn’t involve swallowing pills every day. Some patients just prefer that route, and that’s a valid preference.
- You don’t have brain implants or other conditions that would make TMS unsafe for you. We need to rule those out first, especially when reviewing details whether TMS therapy is covered by insurance and how eligibility is determined.
- Your doctor has already talked with you about whether TMS makes sense for your particular situation. This isn’t something you pursue without that conversation happening.
Practical Guidance for Seeking TMS Treatment
Start by talking with your psychiatrist or primary care doctor about whether TMS might work for your situation. They’ll review your medical history, current symptoms, and treatment attempts to figure out if you’re a candidate. If they think it could help, ask them to recommend providers in your area who offer NeuroStar Advanced TMS Therapy. It’s the FDA cleared system most clinics use.
At TMS of the Carolinas, we handle the technical side of administering the treatment itself.
Our approach centers on precision:
- we map your brain’s motor cortex (the part that controls movement)
- calibrate the magnetic pulse strength to your individual anatomy
- deliver sessions consistently over 4 to 6 weeks.
Most patients come in five days a week for sessions lasting about 37 minutes each.
The insurance piece tends to trip people up, especially when people are already trying to understand TMS therapy costs. We work directly with your insurance company to document medical necessity basically, we show them you’ve tried other treatments first and explain why TMS makes clinical sense for your case.
If coverage gets denied or if you’re uninsured, we offer financing plans so cost doesn’t become the barrier keeping you from treatment.
Your role? Be honest about your symptoms, your past treatments, and what you’re hoping to get out of this. The better your doctor understands your situation, the better they can decide if TMS fits your needs.
FAQ
How does TMS help treatment-resistant depression and why does it show strong TMS efficacy?
TMS sends gentle magnetic pulses to mood areas that are too quiet. This helps those areas fire in a steadier way. Many studies show strong TMS efficacy because the stimulation improves brain balance when medicine isn’t enough.
What should I know about TMS benefits, TMS side effects, and the safety of non-invasive brain stimulation?
TMS benefits include better mood and clearer thinking. Most people return to normal activities right away. TMS side effects are usually mild, like brief tingling or a small headache. Non-invasive brain stimulation has a strong safety record for major depressive disorder.
How do TMS therapy, TMS coil positioning, and TMS brain targeting affect treatment results?
Good TMS coil positioning helps the device reach the dorsolateral prefrontal cortex, a key mood zone. Hitting the right spot improves how well the pulses work. This accuracy supports higher TMS remission rates and a stronger TMS response rate. [2]
How do TMS mechanisms and TMS neuroplasticity guide treatment duration and long-term relapse prevention?
TMS changes brain electrical activity little by little. These changes build neuroplasticity, which strengthens healthier pathways. Treatment lasts weeks so the brain can adjust. Post TMS effects often grow with time, helping lower the chance of relapse later.
Final Thoughts on the Benefits of TMS Therapy
Someone sitting in a waiting room, palms sweating, wondering if there’s actually a way out. That scene plays out quietly for many people living with treatment‑resistant depression, worn down by medications that don’t help enough or bring side effects that feel unbearable. TMS therapy offers a different path.
This treatment uses focused magnetic pulses (similar to those in an MRI) to “wake up” dormant brain synapses, without drugs and without any surgery. It aims at underactive brain areas that help control mood and gently stimulates them so they start working more normally again.
Sessions are brief and structured. Each one can take as little as 19 minutes, usually done five days a week, over about seven weeks. Many patients notice real changes in mood and energy, often within two months, with a stronger ability to take part in daily life again.
Several features make this approach stand out:
- Personalized brain mapping to guide where treatment is aimed
- Minimal side effects for most patients
- Outpatient care, so no hospital stay is needed
During treatment, you stay awake and alert. After each session, you can return to your regular routine the same day.
For people who’ve tried standard treatments without relief, NeuroStar Advanced TMS Therapy may offer the turning point that once felt out of reach.
Ready to explore TMS therapy? Schedule your free consultation at TMS of the Carolinas today
